Now that I have been privileged to witness Doris’s death at her side at home, along with our two children, Eric and Clélia, I am more confident about the hope I expressed earlier that I will be able to greet the moment of my own death like a mother giving birth.
Doris’s journey to death began with what appeared to be a mild stroke in the late afternoon of June 7, 2015. The stroke or its effects only worsened with time, and she moved from the ER to the hospital to rehab to long term care and finally to hospice at home, where she died around eight on Sunday evening July 19th.
At the suggestion of a friend, the family began keeping a journal of these days at CaringBridge.org on the 16th of June. Doris’s pages may be found at this link to CaringBridge. I have used the site’s facilities to make a pdf copy of all the entries there, and this pdf may be downloaded here. (The pdf permits the entries and comments to be read in chronological order on a single web page.)
In retrospect it is easy to see that the family, which was always present, often with grandchildren dancing and playing games or their parents reading chapters of favorite books or me visiting in the morning and feeding her in the refectory in the evening, constantly took a hopeful stance on facts that did not justify the hope. Surely this was not only natural but best for all concerned, and it certainly garnered the support of hospital and care-giving staff all along the line. But it made Doris’s definite decision to die on the evening of July 11th quite shocking.
I came face to face with this when I began the feeding of the evening meal at table with our companions Helen and Marva. I arranged the wheelchair tangentially to our round table and exchanged the usual good-humored banter with Helen – she, like Doris, had suffered a massive stoke disabling the entire right side of her body and her speaking ability back in 2007, but slowly came out of its effects pretty much altogether. Bad luck and bad times for her granddaughter as well as some repeated bouts with pneumonia had brought Helen to the long-term care wing. She always reassured me that Doris was very likely understanding everything that was going on, and in her boldly humorous way would make eyes at Doris, who would smile and even wave feebly in response sometimes. Doris liked Helen, and so did I.
But tonight Doris looked away with fiercely open eyes and deeply down-turned mouth, refusing to recognize Helen and refusing to take any proffered food or drink from me. I thought she was angry, and I thought she was reproaching me for keeping her here in this home, something we had often talked about doing everything we could to avoid. I felt plenty guilty.
The nurse was not able to get Doris to take her meds that evening, and the morning nurse the next day also failed, as I found out when I came in, much concerned. The nurse’s aide who had done special feeding of Doris from the very first over on the rehab side told me she had made every effort, but also failed to feed her breakfast. This story was repeated for mid-day when I came back for the evening feeding and also failed.
But this evening, Sunday the 12th, was different for the presence of a Seventh-Day Adventist missionary volunteer. She was feeding several of the patients tonight as she had the night before. She had talked with me and noticed Doris then. Tonight she approached me at the table and just plain out said, “Your wife has begun the dying process. This is something they do. I’ve seen it many times.”
This event led to my writing the journal entry “Perhaps she’s moving on.” There are questions I do not want to go into now on the topic of why it took a visiting volunteer to tell me what may or may not have been obvious to the nursing and aide staff. While hospice staff confirmed that volunteer’s story, I have not always heard the same things from experienced nursing, aide and hospice care people. And there are interesting physiological questions about how it is even possible for people to live as long as Doris did (eight days without food or drink) or even longer, as one hospice nurse told me. Questions about whether as a couple of our hospice staff told us, administering saline solution to the patient at this time would not only prolong her life but actually cause her pain. A doctor I know denies this is so. And so on.
Letting all that go, I come back to the I-think heroic act of will on Doris’s part that Saturday night when she glared off away from us, fiercely frowning down her mouth, and began to let her body die. This was a powerful woman. And after this, after Sunday evening at least, she slept. With hospice care she lay in a comfortable bed at home instead of being propped in a wheelchair and left sitting with the others at the nurses’ station for the next aide to find or me to show up. In accordance with her wishes as laid out in health directives long ago completed, we offered her no more water or food. Counseled by hospice staff, we properly discarded the dozens and dozens of meds the LTC people sent along with us. And we began to watch with her during her last act of birthing here on Earth. I want to say, birthing her own soul on to another land than ours. It can’t but be a happier one.
The six days lying-in at home were marked on her part almost entirely by sleep and a persistent, restless motion with her left arm and hand – all that she could move. She would pick at the bedclothes at her side, raise her arm rather high in the air and come back to touch her hair a bit with her hand. Then rest, but not long, before repeating these gestures. Eyes closed, breathing at first through her nose, her mouth now even and straight in a soft face. Like this:
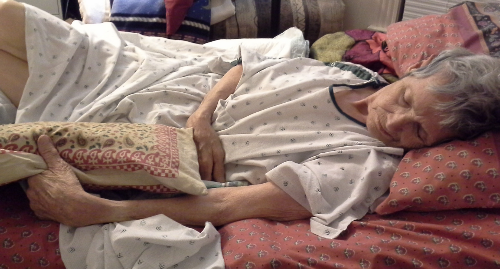
Sometimes she would open her eyes, and then whoever was at bedside with her would call the others and we would wonder at what we saw. For she was not looking at us, and if we put our face in her line of sight, she looked right through us – at what, who can say?
I witnessed two of these brief sessions of looking. They took five or six minutes during which she would shift her gaze from up to the left as we see in the photo above to over to the right. Perhaps two minutes up left and another two up right. Never looking elsewhere, always focused on the ceiling or beyond, never acknowledging us. Just gazing. Solemnly, with great attentiveness, but no fear or other emotion. These looking times had a profound effect on me that I described in the journal entry Whose truth? Whose journey?
The final day and a half, perhaps it was, were marked by rapid breathing and an open mouth with eyes closed. The rate of breathing was quite steady (about thirty times a minute). I had the impression that this was perhaps just her body still on autopilot, her soul having already moved on, but this was not the case as there also came a time very near the end when she lay with her head on the pillow, turned over to her right and her eyes half open. I sat in her line of sight beside the bed and looked into those eyes, thinking she was looking at me, as I at her. But no smile or sign of recognition, just the eyes. And at the last, her head was back in the center, mouth partly open, eyes closed. And the breath would stop, then start again, and then after only a little of this, just stop.
That was five minutes or so before eight in the evening. Clélia had brought the roses the day before –

so she could arrange the body as we discovered it when we came down the next morning:

The coiled-rope phoenix against the wall at the left is a work from Doris’s time with the Tulsa Designer Craftsmen in the 70’s. Here she is with better focus:

These are more or less just the facts. I want to think through the wider meaning of her death for me on the next page. I will extend my thinking in the journal entry noted above,
| The Fifth Remembrance 1 |
| The Fifth Remembrance 2 |
| The Fifth Remembrance 3 |
| Dr. Block and Isys 1 |
| Dr. Block and Isys 2 |
| Dr. Taylor and near death 1 |
| Doris's Death |
| Whose journey? Whose truth? |
| Whose journey? Whose truth? |





